|
Antigen - a foreign substance that causes an immune response in the body
Antibody - a substance produced by the body that fights off antigens Antibiotics - compounds that stop growth in bacteria Monoclonal antibodies - an antibody and a tumour cell combined to clone quickly Hybridoma cells - lymphocytes and tumour cells fused together |
MRSA - methicillin-resistant staphylococcus aureus
Influenza - flu virus Vaccination - injection of a weakened or mild form of a pathogen to produce immunity Immune - protected from a disease Pathogen - an organism that causes disease |
Antibody Drugs
|
Tetracycline Interactions
Tetracycline + Isotretioin
Threshold of toxicological concern TTC ADRs adverse drug reaction
Doxycycline
Minocycline Acne |
Erythromycin ADRs
Activate motilin receptors which increases peristalsis Azithromycin Coverage
Clarithromycin Coverage Tends to be mostly for H. pylori coverage Azithromycin
Fidaxomicin ADRs
|
Cell-mediated immunity
-after being activated in response to an antigen, helper T cells will release of cytokines that activate cytotoxic T cells, natural killer cells, macrophages, granulocytes, and B cells
-specifically, helper T cells release cytokines that induce the transformation of B cells to plasma cells, the latter of which can secrete antibodies to fight infection
How the type of antigen presenting cell affects the outcome of an immune response
-antigen presentation by dendritic cells or activated macrophages that express high levels of MHC class II and co-stimulatory molecules results in highly effective activation of T cells
-antigen presentation by "non-professional" antigen presenting cell that do not express co-stimulatory molecules results in little or no activation of T cells
-adjuvants facilitate immune responses by inducing the expression of high levels of MHC and co-stimulatory molecules
Antibody activation
-the cross-linking of surface immunoglobulins leads to the activation of the B cell
-the binding of an antigen to two or more antibodies on an antigen presenting cell will induce conformational changes in the fraction of crystallization that induce an immune response
-note that the activation of "like" receptors cause activation of the immune response
Antibody blocking
-occurs when high levels of the antibody IgG are present, resulting in competition for binding to surface immunoglobulins
-the competing antibodies must be high affinity and recognize the same epitope (i.e. independent of the fraction of crystallization)
Cross-linking of "unlike" receptors
-a form of antibody blocking that involves the binding of two different epitopes to two different immunoglobulins located on a B cell
-leads to the production of conflicting signals
-prevents the B cell from being activated as there is already enough antibody present to fight the infection
Anti-iditotypic antibodies
-antibodies that specifically bind to the epitope binding site of another antibody
-generated through the recombination/mutation of genes that code for the epitope binding site
-can dampen the immune response by removing antibodies through the formation of immune complexes and the cross-linking of "unlike" receptors
-can increase reactivity to a specific antigen to the cross-linking of surface immunoglobulins
-can cause increased antigen uptake to increase antigen processing and presentation through fraction of crystallization receptors or surface immunoglobulins
Differentiation of helper T cells
-once an immature helper T cell differentiates into a TH0 cell, it will acquire a variety of genes that can be expressed to synthesize a variety of proteins
-in response to the cytokines in the surrounding environment, TH0 cells can subsequently differentiate into a variety of TH cells
-this differentiation of the TH0 cells involves represses the expression of particular genes so only certain proteins can be synthesized
How peptide density/binding affinity to MHC class II affects the differentiation of helper T cells
-high affinity to MHC class II favors the differentiation of helper T cells so they produce TH1 responses
-low affinity to MHC class II favors the differentiation of helper T cells so they produce TH2 responses
TH1 helper T cells
-secretes cytokines including IFN-γ, TNF-β and IL-2
-promotes the activation of macrophages, antibody-dependent cell-mediated cytotoxicity, and delayed-type hypersensitivity
-IL-2 inhibits responses from TH2 helper T cells
TH2 helper T cells
-secretes cytokines including IL-4, IL-5, IL-6, IL-9, IL-10, and IL-13
-promotes antibody responses, IgG and IgE isotype switching, the stimulation of mast cell/eosinophil growth and differentiation, and the synthesis of IgA
-IL-10 inhibits responses from TH1 helper T cells
-after being activated in response to an antigen, helper T cells will release of cytokines that activate cytotoxic T cells, natural killer cells, macrophages, granulocytes, and B cells
-specifically, helper T cells release cytokines that induce the transformation of B cells to plasma cells, the latter of which can secrete antibodies to fight infection
How the type of antigen presenting cell affects the outcome of an immune response
-antigen presentation by dendritic cells or activated macrophages that express high levels of MHC class II and co-stimulatory molecules results in highly effective activation of T cells
-antigen presentation by "non-professional" antigen presenting cell that do not express co-stimulatory molecules results in little or no activation of T cells
-adjuvants facilitate immune responses by inducing the expression of high levels of MHC and co-stimulatory molecules
Antibody activation
-the cross-linking of surface immunoglobulins leads to the activation of the B cell
-the binding of an antigen to two or more antibodies on an antigen presenting cell will induce conformational changes in the fraction of crystallization that induce an immune response
-note that the activation of "like" receptors cause activation of the immune response
Antibody blocking
-occurs when high levels of the antibody IgG are present, resulting in competition for binding to surface immunoglobulins
-the competing antibodies must be high affinity and recognize the same epitope (i.e. independent of the fraction of crystallization)
Cross-linking of "unlike" receptors
-a form of antibody blocking that involves the binding of two different epitopes to two different immunoglobulins located on a B cell
-leads to the production of conflicting signals
-prevents the B cell from being activated as there is already enough antibody present to fight the infection
Anti-iditotypic antibodies
-antibodies that specifically bind to the epitope binding site of another antibody
-generated through the recombination/mutation of genes that code for the epitope binding site
-can dampen the immune response by removing antibodies through the formation of immune complexes and the cross-linking of "unlike" receptors
-can increase reactivity to a specific antigen to the cross-linking of surface immunoglobulins
-can cause increased antigen uptake to increase antigen processing and presentation through fraction of crystallization receptors or surface immunoglobulins
Differentiation of helper T cells
-once an immature helper T cell differentiates into a TH0 cell, it will acquire a variety of genes that can be expressed to synthesize a variety of proteins
-in response to the cytokines in the surrounding environment, TH0 cells can subsequently differentiate into a variety of TH cells
-this differentiation of the TH0 cells involves represses the expression of particular genes so only certain proteins can be synthesized
How peptide density/binding affinity to MHC class II affects the differentiation of helper T cells
-high affinity to MHC class II favors the differentiation of helper T cells so they produce TH1 responses
-low affinity to MHC class II favors the differentiation of helper T cells so they produce TH2 responses
TH1 helper T cells
-secretes cytokines including IFN-γ, TNF-β and IL-2
-promotes the activation of macrophages, antibody-dependent cell-mediated cytotoxicity, and delayed-type hypersensitivity
-IL-2 inhibits responses from TH2 helper T cells
TH2 helper T cells
-secretes cytokines including IL-4, IL-5, IL-6, IL-9, IL-10, and IL-13
-promotes antibody responses, IgG and IgE isotype switching, the stimulation of mast cell/eosinophil growth and differentiation, and the synthesis of IgA
-IL-10 inhibits responses from TH1 helper T cells
|
Pathogenic conversion of regulatory B10 cells into osteoclast-priming cells in rheumatoid arthritis
Fanle Hua,et al. Journal of Autoimmunity Volume 76, January 2017, Pages 53-62 https://www.sciencedirect.com/science/article/abs/pii/S089684111630141X Collectively, these results showed that in RA, regulatory B10 cells demonstrated the potential of converting into RANKL-producing cells, thus exacerbating osteoclast formation, bone destruction and disease progression. Modulating the status of B10 cells might provide novel therapeutic strategies for RA. |
Highlights
•Regulatory B10 cells were functionally impaired in RA patients . •Under RA circumstance, regulatory B10 cells demonstrated the potential of converting into RANKL-producing cells . •RANKL-producing B10 cells expanded dramatically in RA patients and were positively correlated with the disease activities . •RANKL-producing B10 cells from RA patients significantly promoted osteoclast differentiation and bone erosion . •RANKL-producing B10 cells declined while regulatory B10 cells increased in RA patients with remission after therapy . |
|
|
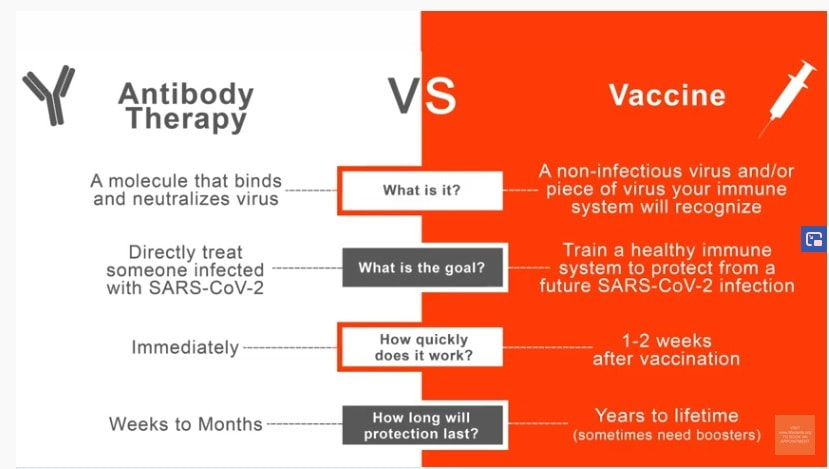
How is Monoclonal Antibody Therapy different from COVID vaccines?
|
Dr Arvinder S Soin, Chairman, Institute of Liver Transplant and Regenerative Medicine at Medanta Hospital pushed for production of Monoclonal antibody drug in India. Soin said availability of the drug in India at a reasonable price could be a game changer for the country in its fight against Covid-19. Soin said, “There are three specific drugs in the form of monoclonal antibodies against the viral spike protein that have been authorised for emergency use by the US FDA, and one by the CDSCO, India. These can nip Covid infection in the bud, if given soon after testing positive but certainly in the first week.” Watch the full video for more.
|
Paragraph. ここをクリックして編集する.
|
Self Tolerance and Microbe Triggered Autoimmunity (T Cell Focus)
www.youtube.com/watch?v=oCce3IrL3fA |
Receptor type protein tyrosine phosphatases (RPTPs) – roles in signal transduction and human disease
https://www.ncbi.nlm.nih.gov
Protein tyrosine phosphorylation is a fundamental regulatory mechanism controlling cell proliferation, differentiation, communication, and adhesion. Disruption of this key regulatory mechanism contributes to a variety of human diseases including cancer, diabetes, and auto-immune diseases. J Cell Commun Signal. 2012 Aug; 6(3): 125–138.
https://www.ncbi.nlm.nih.gov
Protein tyrosine phosphorylation is a fundamental regulatory mechanism controlling cell proliferation, differentiation, communication, and adhesion. Disruption of this key regulatory mechanism contributes to a variety of human diseases including cancer, diabetes, and auto-immune diseases. J Cell Commun Signal. 2012 Aug; 6(3): 125–138.
Population-based estimates of humoral autoimmunity from the U.S. National Health and Nutrition Examination Surveys, 1960-2014 - PubMed (nih.gov)
NHANES III data show that the overall US prevalence of having a detectable serum autoantibody is substantial in adults, in both women and men.
NHANES III data show that the overall US prevalence of having a detectable serum autoantibody is substantial in adults, in both women and men.
- Thyroid autoantibodies were present in 18% of US adults (31 million persons) including 10% of younger adults and 25% of older persons.
- Overall autoantibody prevalences increased significantly with age: 32% of US adults 60+ years of age (12.8 million persons) had at least one of the four autoantibodies rheumatoid factor, anti-thyroglobulin, anti-thyroperoxidase, or anti-tissue transglutaminase.
- Older women had higher levels of autoantibodies, but this was a relative difference.
- Autoantibody prevalence in both sexes was substantial (women 39%; men 22%). Fourteen percent of adults 60+ years of age have multiple autoantibodies.
Antibodies
|
Antibody to Antigen Relationship
|
HLA-B27
ankylosing spondylitis 88% HLA-B27 human leucocyte antigen HLA-B27 Reactive arthritis 50-60% HLA-B27 psoriatic arthritis 60-70% HLA-B27 IBD coeliac disease immunoglobulin IgA |
coeliac disease
1) Anti-tissue transglutaminase antibodies (IgA), anti-tTG 2) Anti-endomysial antibody (IgA) (EMA) 3) Anti-deamidated dliafin peptides (IgG), Biliary Cirrhosis Antimitrochondrial antibodies, (IgM) 95% Anti-mitochondrial antibodies, IgM, 95% biliary cirrhosis anti-smooth muscle 95% PBC, IgG |
Antibodies against N or S protein were correlated with neutralizing antibody titers, which may be useful when screening convalescent plasma for passive transfusion therapy. https://www.jci.org/articles/view/138759
|
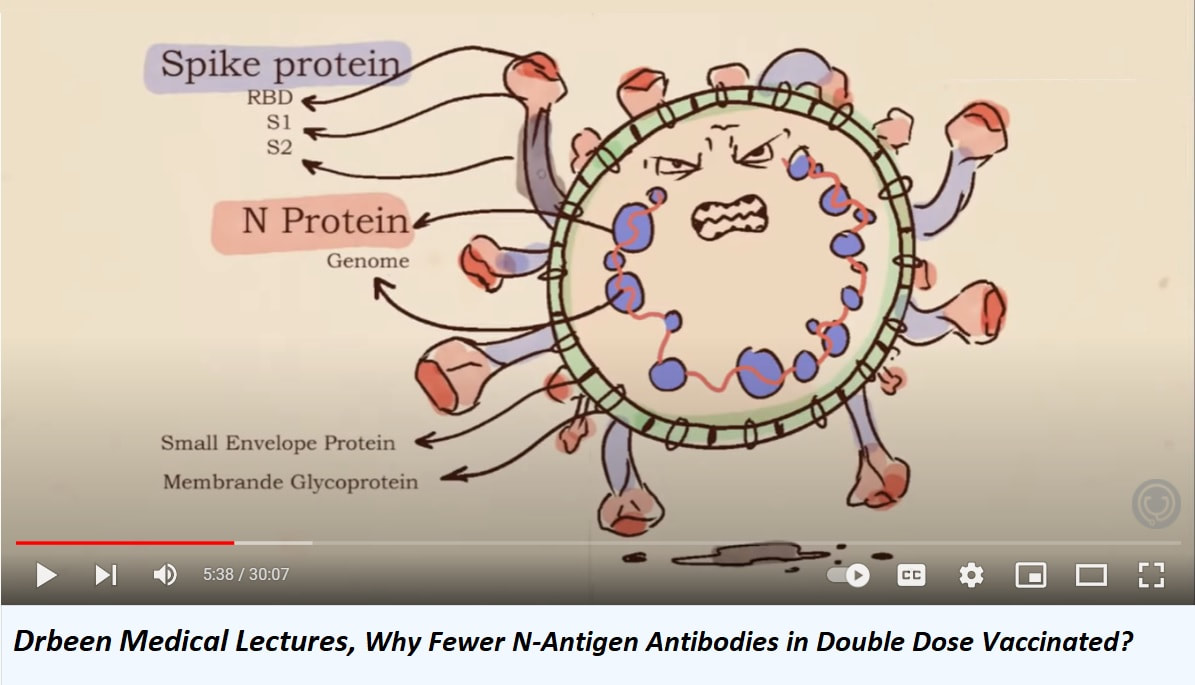
N protein
|
S protein
|
|
Characterization and application of monoclonal antibodies against N protein of SARS-coronavirus Bo Shang, et al.,
www.ncbi.nlm.nih.gov/pmc/articles/PMC7092910/ Drbeen Medical Lecture, https://www.youtube.com/channel/UCrtd2wePvAl6RN_D-9jWVQQ "Why Fewer N-Antigen Antibodies in Double Dose Vaccinated?" |
www.youtube.com/watch?v=C4ERVQV4s5s&t=5s
CoV-2 can also serve as an important target for the development of potent and specific nAbs. Cocktails comprising antibodies specific for RBD and other regions in the S protein may further improve the breadth and potency of nAbs against SARS-CoV-2 and its escape-mutant strains. Human sera from convalescent patients have been used to treat COVID-19, but lessons learned from SARS show that some non-nAbs targeting the non-RBD regions in the S protein may cause an antibody-dependent enhancement (ADE) effect on viral infectivity and disease, as well as other harmful immune responses [2]. www.sciencedirect.com/science/article/pii/S1471490620300570 |
Autoantibody https://en.wikipedia.org/wiki/Autoantibody
- Indications for autoantibody tests
- Antibody profiling
- List of some autoantibodies and commonly associated diseases (Rheumatoid factor IgG, anti-CCP, cyclic citrullinated peptide , rheumatoid arthritis )
|
Production
Antibodies are produced by B cells in two ways: (i) randomly, and (ii) in response to a foreign protein or substance within the body. Initially, one B cell produces one specific kind of antibody. In either case, the B cell is allowed to proliferate or is killed off through a process called clonal deletion. Normally, the immune system is able to recognize and ignore the body's own healthy proteins, cells, and tissues, and to not overreact to non-threatening substances in the environment, such as foods. Sometimes, the immune system ceases to recognize one or more of the body's normal constituents as "self," leading to production of pathological autoantibodies. Autoantibodies may also play a nonpathological role; for instance they may help the body to destroy cancers and to eliminate waste products. The role of autoantibodies in normal immune function is also a subject of scientific research. |
Cause
The causes of autoantibody production are varied and not well understood. It is thought that some autoantibody production is due to a genetic predisposition combined with an environmental trigger, such as a viral illness or a prolonged exposure to certain toxic chemicals. There is generally not a direct genetic link however. While families may be susceptible to autoimmune conditions, individual family members may have different autoimmune disorders, or may never develop an autoimmune condition. Researchers believe that there may also be a hormonal component as many of the autoimmune conditions are much more prevalent in women of childbearing age. While the initial event that leads to the production of autoantibodies is still unknown, there is a body of evidence that autoantibodies may have the capacity to maintain their production.[1][2] |
Diseases
The type of autoimmune disorder or disease that occurs and the amount of destruction done to the body depends on which systems or organs are targeted by the autoantibodies, and how strongly. Disorders caused by organ specific autoantibodies, those that primarily target a single organ, (such as the thyroid in Graves' disease and Hashimoto's thyroiditis), are often the easiest to diagnose as they frequently present with organ related symptoms. Disorders due to systemic autoantibodies can be much more elusive. Although the associated autoimmune disorders are rare, the signs and symptoms they cause are relatively common. Symptoms may include: arthritis-type joint pain, fatigue, fever, rashes, cold or allergy-type symptoms, weight loss, and muscular weakness. Associated conditions include vasculitis which are inflammation of blood vessels and anemia. ... |
Receptor type protein tyrosine phosphatases (RPTPs) – roles in signal transduction and human disease
www.ncbi.nlm.nih.gov/pmc/articles/PMC3421019/ J Cell Commun Signal. 2012 Aug; 6(3): 125–138.
Proposed biologic functionsIA2 is a major auto-antigen in type I diabetes (Notkins 2002). Approximately 70 % of newly diagnosed type I diabetes patients have auto-antibodies to IA2 (Lan et al. 1996). These auto-antibodies appear years before the onset of clinical symptoms. Approximately 50 % of subjects who display auto-antigens to both IA2 and GAD65 (a glutamic acid decarboxylase identified as another major type I diabetes auto-antigen) will develop type I diabetes within 5 years (Hu et al. 2005). Therefore, IA2 auto-antibody screening is now widely used to enrich trial enrollment for clinical studies of type I diabetes interventions.
www.ncbi.nlm.nih.gov/pmc/articles/PMC3421019/ J Cell Commun Signal. 2012 Aug; 6(3): 125–138.
Proposed biologic functionsIA2 is a major auto-antigen in type I diabetes (Notkins 2002). Approximately 70 % of newly diagnosed type I diabetes patients have auto-antibodies to IA2 (Lan et al. 1996). These auto-antibodies appear years before the onset of clinical symptoms. Approximately 50 % of subjects who display auto-antigens to both IA2 and GAD65 (a glutamic acid decarboxylase identified as another major type I diabetes auto-antigen) will develop type I diabetes within 5 years (Hu et al. 2005). Therefore, IA2 auto-antibody screening is now widely used to enrich trial enrollment for clinical studies of type I diabetes interventions.
Autoantibodies to islet antigen-2 are associated with HLA-DRB1*07 and DRB1*09 haplotypes as well as DRB1*04 at onset of type 1 diabetes: the possible role of HLA-DQA in autoimmunity to IA-2
Paragraph. ここをクリックして編集する.